DRY MOUTH (XEROSTOMIA) IN SMOKERS AND ALCOHOL USERS: CAUSES, RISKS & SOLUTIONS
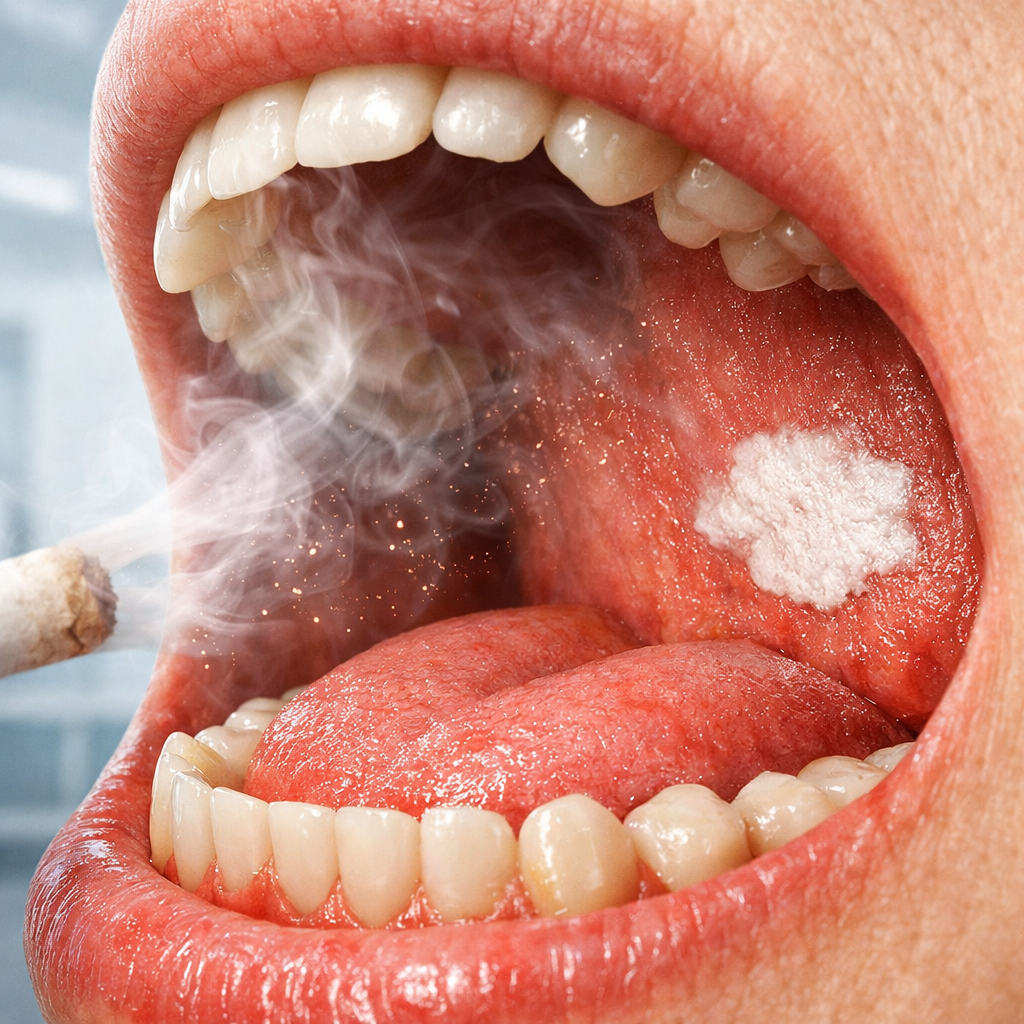
DRY MOUTH (XEROSTOMIA) IN SMOKERS AND ALCOHOL USERS: CAUSES, RISKS & SOLUTIONS What is Dry Mouth? Dry mouth, medically known as xerostomia, occurs when saliva production decreases. Saliva is not just moisture — it is protective fluid containing enzymes, antibodies, and buffering agents. Smoking and alcohol both reduce saliva production. Nicotine affects salivary gland signaling, while alcohol dehydrates tissues. Why Saliva Is Essential Saliva plays critical roles: Neutralizes acids Washes away food debris Maintains mucosal lubrication Supports tissue healing When saliva decreases, the oral lining becomes: Rough Sensitive More prone to irritation Susceptible to infection Persistent dryness can also alter taste perception and make chewing uncomfortable. Lifestyle-Related Xerostomia Smokers often wake up with dry mouth. Alcohol users experience dehydration-related dryness. Tobacco chewers may develop localized dryness where the pouch is placed. Chronic dryness contributes to: Burning mouth sensation White patches Micro-cracks in mucosa Increased oxidative stress Supporting Oral Moisture & Tissue Integrity Hydration is important, but hydration alone may not restore mucosal resilience. Supporting the epithelial barrier and antioxidant balance may help improve comfort. How BOYA10 May Support Oral Comfort When chewed, BOYA10 forms a thin coating layer over the mucosa. This coating: Enhances localized contact Supports mucosal barrier integrity Provides antioxidant support Helps maintain epithelial resilience By acting before swallowing, BOYA10 focuses on the first site affected by dryness. 👉 Learn more:https://BOYA10.com/faqs
DRY MOUTH (XEROSTOMIA) IN SMOKERS AND ALCOHOL USERS: CAUSES, RISKS & SOLUTIONS Read More »