THE ORAL-SYSTEMIC HEALTH CONNECTION: HOW LIFESTYLE HABITS IMPACT THE ENTIRE BODY
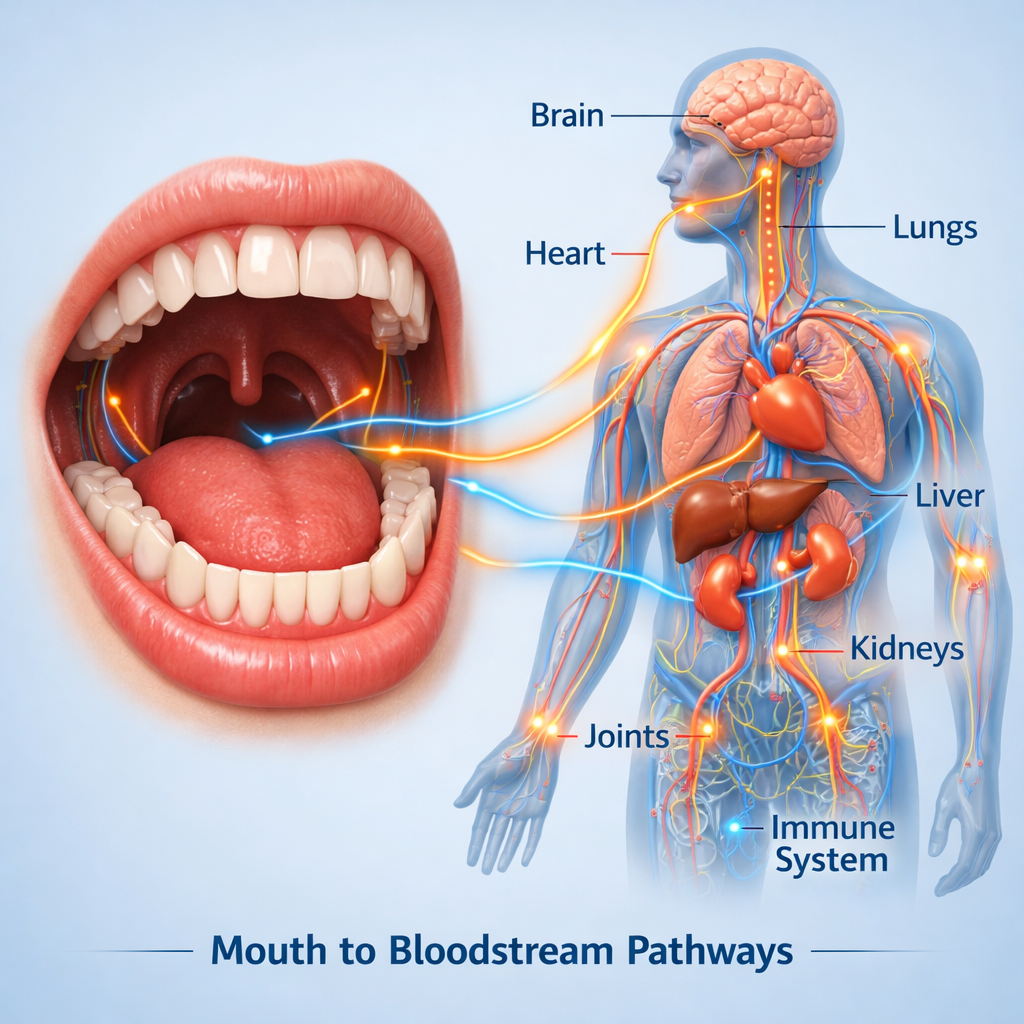
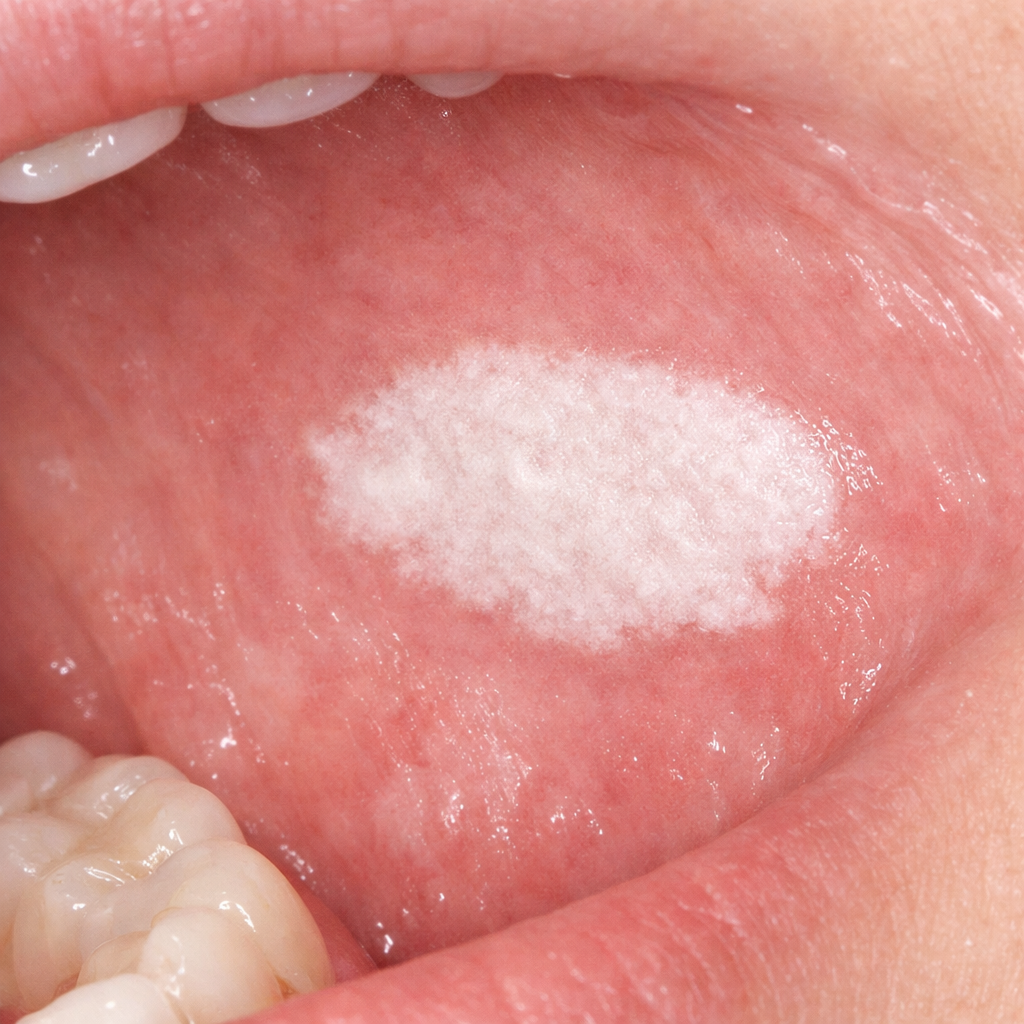
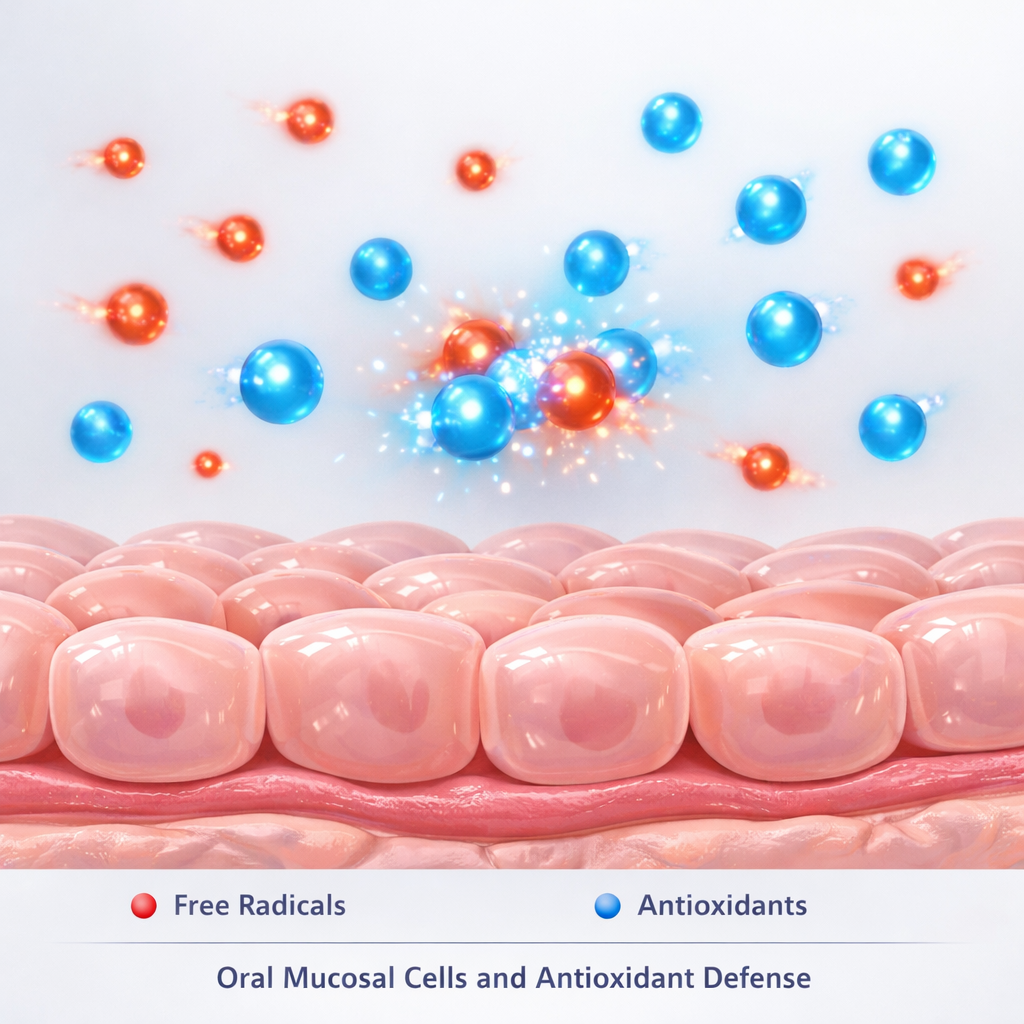
THE ORAL-SYSTEMIC HEALTH CONNECTION: HOW LIFESTYLE HABITS IMPACT THE ENTIRE BODY The Mouth as a Gateway The oral cavity is connected to the digestive and circulatory systems. Substances absorbed through oral mucosa can enter bloodstream rapidly. Smoking, tobacco chewing, and alcohol exposure not only affect oral tissues but may influence systemic health markers. Oral Inflammation and Systemic Impact Chronic irritation in the mouth can trigger inflammatory mediators. Emerging research suggests links between oral health and: Cardiovascular health Immune response balance Metabolic function While direct causation varies, maintaining oral tissue integrity is part of broader wellness. Supporting Local and Systemic Health Because the mouth is the first site of exposure, targeted local support may be beneficial. BOYA10 Dual-Phase Concept BOYA10 is unique because it: Acts locally inside the mouth before swallowing Provides continued internal nutritional support This dual-phase design bridges oral and systemic wellness support in a structured manner. For individuals with high-risk lifestyle habits, this integrated approach may complement broader health strategies. 👉 Explore more:https://BOYA10.com/ingredientshttps://BOYA10.com/faqs
THE ORAL-SYSTEMIC HEALTH CONNECTION: HOW LIFESTYLE HABITS IMPACT THE ENTIRE BODY Read More »